
VETERAN POST TRAUMATIC STRESS DISORDER & GROWTH
IN COVID-19
Ahalya Ramesh
INTRODUCTION
Although the prevalence of PTSD among veterans is largely disputed - varying across wars and sources - there is a consensus that veterans are disproportionately affected compared to the general public. However, less than half receive any form of treatment; veterans consistently cite a fear of being considered weak for seeking mental health treatment, discomfort with existing resources within the Department of Veterans Affairs (VA) or Department Of Defense (DOD), and inconsistent treatment due to busy personal schedules, long waiting lists at the VA and switching providers as barriers to accessing such services. These barriers have only been amplified by COVID-19, with the VA, nonprofits, and other service providers transitioning to digital platforms. Moreover, given that the strongest predictive tool for the development of PTSD is the lifetime trauma load - an unweighted sum score of one’s net trauma exposures - the additive effects of COVID-19 related trauma and war-related trauma position veterans as uniquely vulnerable subjects in the face of a pandemic.
The following project synthesizes the extensive research that has documented the negative psychological consequences of COVID-19 and juxtaposes it with ideas of resilience. That is, it explores a gap in the literature on any salutogenic effects or positive psychological changes onset by the pandemic. By grappling with the bifurcation of trauma, it suggests that COVID-19 has not only exacerbated PTSD symptomology in veterans, but also facilitated resilience and post-traumatic growth (PTG) in the form of an increased appreciation for life, improved interpersonal relationships, feelings of increased personal strength, positive spiritual changes, or new meaning and purpose in life.
HOW ARE VETERANS WITH PTSD INCREASINGLY RESILIENT
IN THE FACE OF COVID-19?
HOW ARE VETERANS WITH PTSD INCREASINGLY VULNERABLE IN THE FACE OF COVID-19?
MIXED METHODS APPROACH
SURVEY FINDINGS

Source: Getty Images
Survey Data
A Synthesis of existing data on PTG and PTSD during COVID-19

Source: Rocky Mountain Regional VA Medical Center, taken by Hyong Chang for Denver Post
Expert Opinions
Perspectives from physicians, service providers, and nonprofits

Source: Interviewee Sergio Alfaro, taken by Jenna Schoenfeld for NBC News
Veteran Interviews
A review of published veteran narratives taken during COVID-19
Quantifying the COVID-19 Quality of Life Burden:
-
Veterans diagnosed with PTSD (based on the PCL-5 scale) are 3.21x more likely to suffer a larger COVID-19 quality of life burden. This makes PTSD a RISK FACTOR.
-
Veterans with a higher resiliency score (based on the CD-RISC 10 scale) are 55% less likely to suffer a larger COVID-19 quality of life burden. This distinguishes resiliency as a PROTECTIVE FACTOR.
Call volumes to the Veterans Crisis Line increased by 15% in the past year, representative of a broader upwards trend in veteran treatment-seeking behavior:

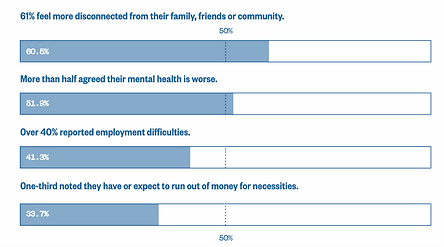
Social distancing has had a substantial negative impact on veteran wellbeing:
Veteran Small Business Owners show resilience financially:
-
Despite 65% of veteran small business owners self-reporting that COVID-19 continues to negatively impact their business, veterans have fared considerably better (a 10-15% difference) in reopening their small businesses, maintaining cash reserves, and paying their rent in full and on time than their counterparts.
"Veteran business owners are battle-tested and accustomed to overcoming adversity and difficult circumstances. They’re trained to survive in the worst of situations.”
- Veteran business owner Jerry Bowden
Clinically, veterans with PTSD have better health outcomes related to COVID-19:
-
Veterans with PTSD are more likely to be tested and less likely to test positive for COVID-19 than veterans without PTSD. This is due to their persisting PTSD symptomatology - namely hypervigilance, avoidance, and increased social isolation.
Prior to COVID-19, veterans, and even more so veterans with PTSD, have been proven to express greater signs of post-traumatic growth than the general population. A follow-up study comparing PTG levels from 2019-2020 to COVID times found that just one year into the pandemic, 43.3% of veterans report moderate or great levels of COVID-19 related post-traumatic growth. More importantly, veterans who screened positive for COVID-19 related symptoms of PTSD exhibited a significantly higher prevalence of post-traumatic growth, 71.9%, compared to veterans without PTSD.
These results call for a critical reevaluation of frames that conceptualize post-traumatic growth and post-traumatic stress disorder as mutually exclusive.
EXPERT PERSPECTIVES
“Isolation is one of the symptoms of PTSD and it is extremely difficult to help a veteran who is struggling to reach out. Not being able to stay connected physically can lead to greater depression and despair.”
- Michelle McMillen, an executive at the PTSD Foundation of America
The “deployment-mind” is uniquely equipped with:
-
Experience in putting the collective good above personal freedom
-
Training to cope with crisis
-
Adapting to adversity
-
Avoidance
-
Hypervigilance
